Stress and autoimmunity: understanding the connection
 Stress isn’t just something that affects your mood—it can have a major impact on your physical health too. In fact, stress can play a role in triggering autoimmune diseases, where the body’s immune system mistakenly attacks its own healthy cells. Let’s break down how stress can lead to autoimmunity.
Stress isn’t just something that affects your mood—it can have a major impact on your physical health too. In fact, stress can play a role in triggering autoimmune diseases, where the body’s immune system mistakenly attacks its own healthy cells. Let’s break down how stress can lead to autoimmunity.
How stress affects the body
When you’re stressed, your body reacts through several systems working together: your nervous system (which controls your brain and nerves), your endocrine system (which manages hormones), and your immune system (which defends against illness). Here’s how they get involved:
1. Neuroendocrine dysregulation: When stress hormones take over
When you feel stressed, your body sounds the alarm through something called the hypothalamic-pituitary-adrenal (HPA) axis. Think of it like your body’s emergency response system. This triggers:
• Release of stress hormones: Your body releases hormones like cortisol (known as the “stress hormone”) and adrenaline. These hormones help in short bursts, like when you need to react quickly in an emergency. But if stress sticks around too long, these hormones can throw your body out of balance.
• Cytokine imbalance: Cytokines are messengers that help your immune system respond to infections and injuries. Stress messes with these signals, causing too many inflammatory messages and not enough calming ones.
• Immune cell disruption: Stress can confuse your immune system, making some cells overactive while others become sluggish. This imbalance can lead your body to mistakenly attack itself.
2. Immune system alterations: Turning up the inflammation
When stress becomes chronic (lasting weeks, months, or even years), it can change how your immune system works:
• Increased inflammation: Your body produces more substances called pro-inflammatory cytokines (like IL-6 and TNF-α). While inflammation helps fight infections, too much can damage healthy tissues.
• Reduced anti-inflammation: Your body makes fewer calming cytokines (like IL-10), which normally keep inflammation in check.
• Trouble with cortisol: Usually, cortisol helps control inflammation. But with constant stress, your body stops responding to cortisol properly, allowing inflammation to spiral out of control.
3. Molecular mimicry: When your body gets confused
Sometimes stress causes changes in your body that confuse the immune system:
• Altered self-antigens: Stress can change the way your body’s own cells look to the immune system. The immune system may start to think these normal cells are invaders.
• Mistaken identity: The immune system may create antibodies (proteins that fight infections) that accidentally attack healthy cells because they look too similar to harmful invaders. It’s like mistaking a friend for a stranger because they’re wearing a disguise.
4. Intestinal barrier dysfunction: The leaky gut problem
Your gut isn’t just for digestion—it also plays a huge role in your immune health. Stress can affect your gut in harmful ways:
• Leaky gut: Stress can weaken the lining of your intestines, creating tiny gaps that allow bacteria, toxins, and undigested food particles to “leak” into the bloodstream. This is called increased intestinal permeability.
• Immune overreaction: When these foreign substances enter the bloodstream, the immune system goes on high alert, leading to chronic inflammation and potentially triggering autoimmune responses.
5. Epigenetic modifications: Stress changing your genes
While stress doesn’t change your DNA, it can influence how your genes work:
• Gene regulation changes: Stress can switch certain genes on or off, especially those related to the immune system. This can make your body more prone to inflammation.
• DNA methylation: Stress can add or remove chemical tags on your DNA (a process called methylation), changing how genes are expressed. This can lead to immune system problems over time.
6. Psychological factors: The mind-body connection
Stress doesn’t just affect you physically—it also impacts your behaviour and mental health, which can further influence autoimmune conditions:
• Unhealthy coping mechanisms: Chronic stress may lead to habits like poor diet, lack of sleep, smoking, or drinking too much alcohol—all of which can weaken the immune system.
• Worsening symptoms: If you already have an autoimmune condition, stress can trigger flare-ups, making symptoms worse and harder to manage.
What the research says
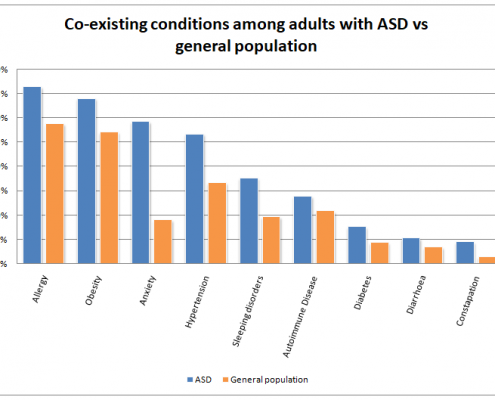
Studies show that up to 80% of people report experiencing major emotional stress before developing an autoimmune disease. This doesn’t mean stress is the only cause, but it’s often a significant trigger when combined with other factors like genetics and environment.
It’s not just about stress
Autoimmune diseases are complex and usually happen due to a combination of things:
• Genetic predisposition: Some people are more likely to develop autoimmune diseases because of their family history.
• Environmental triggers: Things like infections, toxins, and diet can play a role.
• Lifestyle factors: Lack of exercise, poor sleep, and chronic stress can all increase risk.
Taking control: How to manage stress and reduce risk
While you can’t change your genes, you can control how you manage stress. Some helpful strategies include:
• Mindfulness and meditation: Practices that help calm the mind and reduce stress.
• Physical activity: Regular exercise helps regulate stress hormones and boost mood.
• Healthy diet: Eating nutritious foods supports both mental and immune health.
• Therapy or counselling: Talking to a professional can help manage emotional stress.
Book your nutritional therapy appointment
Ready to explore a tailored approach? Book a free 20-minute inquiry call today and let’s work together on a path to better health.